Fentanyl for labour pain management: a scoping review. BMC Pregnancy Childbirth. 2022; 22: 846.
Drugs and Lactation Database (LactMed®) [Internet]. Last Revision: February 15, 2023.
Liposomal bupivacaine (Exparel) is a longer acting form of traditional bupivacaine that delivers the drug by means of a multivesicular liposomal system.

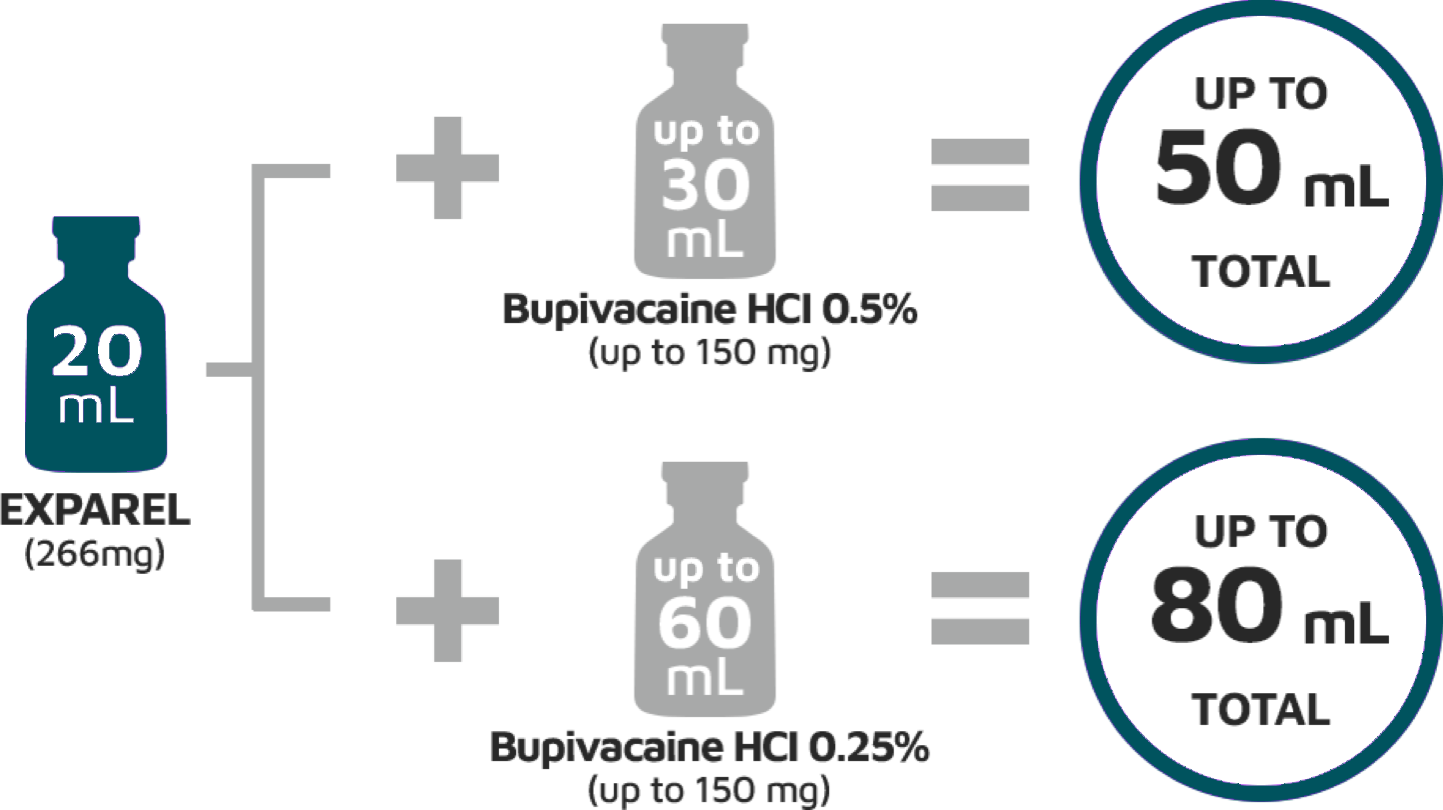
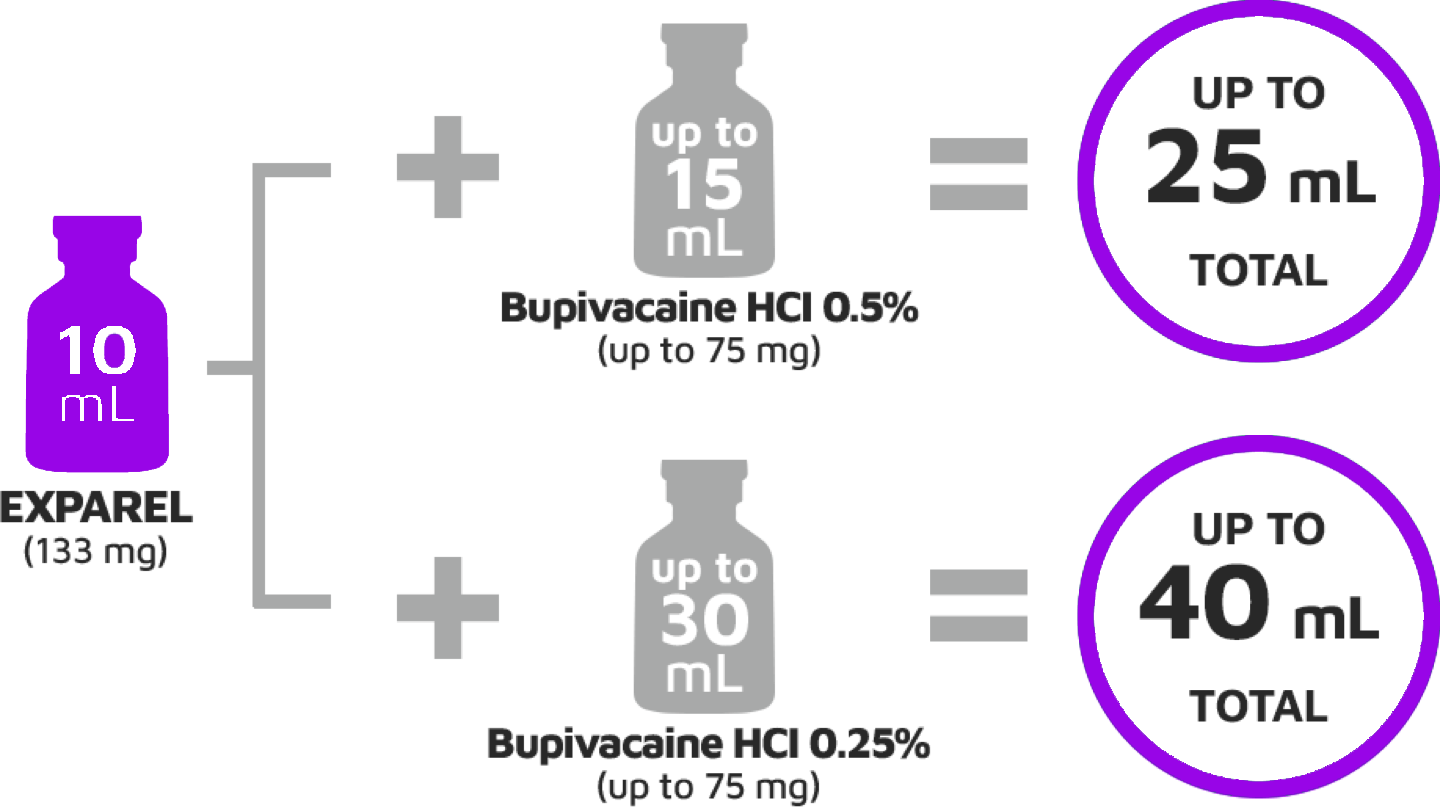
Exparel dosing company info: Pocket Dosing Guide , Billing Guide
Liposomal bupivacaine: a review of a new bupivacaine formulation. J Pain Res. 2012; 5: 257–264.
Rib fractures case report: ESP block
20-something year old primip came today with preeclampsia and was deemed a c/s candidate for her 26 week baby. She was 5’8″, 165lb and had no prior issue with previous surgeries. She was started on magnesium preop. The mag was held intraoperatively and would resume postoperatively. Pt was in sitting position for her spinal, which was placed at L4-5. Good clear CSF return. 0.75% bupi dosed at 13.5 mg with intrathecal fentanyl 15mcg and intrathecal morphine 0.2mg. BP decreased from 150s to 130s, which was appropriate. Patient stated she had increased tingling and decreased mobility in her legs. All symptoms and signs appropriate with her spinal. Patient passed the Allis clamp test prior to incision. She was quite anxious: propofol was given IV for anxiolysis. Patient was adamant about breastfeeding/pumping for her baby. No complications with delivery. Uterus was externalized and patient was sensitive to pressure and tugging/manipulation. IV fenatnyl and IV morphine were given along with IV propofol. When uterus was internalized, patient felt more pressure that seemed unbearable. More IV pain meds were given. Suggestion was made for intraperitoneal chloroprocaine. Patient able to tolerate fascial closure as well as staple skin closure.
Pain Control During Cesarean Delivery. Anesthesia Experts. Jan 2020.


Update: April 2023



Perioperative Dexmedetomidine Improves Outcomes of Cardiac Surgery. Circulation. 2013;127:1576–1584.
I’ve done a good deal of research on the benefits of an ERAS and Cardiac ERAS protocol to help with decreased length of hospital stay as well as early extubations and perioperative adjuvant pain control with ketamine, methadone, regional anesthesia, adjuvants to regional, etc.

Methadone: perioperative use; acute and chronic pain
Updates on Multimodal Analgesia for Orthopedic Surgery. Anesthesiol Clin. 2018 Sep;36(3):361-373.
Regional for Cardiothoracic Anesthesia
Gathering data for Cardiac ERAS program for our hospital as well as the SCA. This page will be continuously updated as I find more information.




Review: Thoracic Paravertebral Block. Anesthesiology. Sept 2001.
Ultrasound-Guided Paravertebral Block Anaesthesia Tutorial of the Week. April 2018. Tutorial #376.

YouTube: PVB catheter technique
YouTube: U/S-guided PVB by Block Jocks
YouTube: nerveblocks U/S-guided PVB
YouTube: thoracic PVB and anatomy
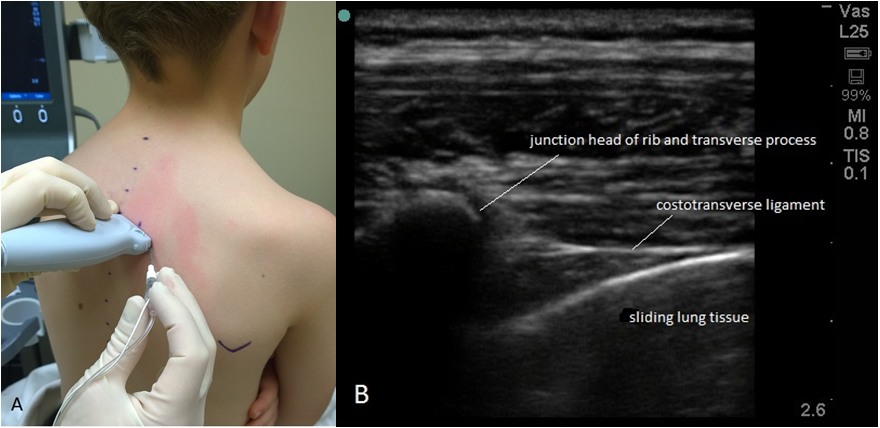
Nov 2021:
https://www.sciencedirect.com/science/article/pii/S1053077020300987?via%3Dihub
Continuous paravertebral block using a thoracoscopic catheter-insertion technique for postoperative pain after thoracotomy: a retrospective case-control study. Journal of Cardiothoracic Surgery volume 12, Article number: 5 (2017)
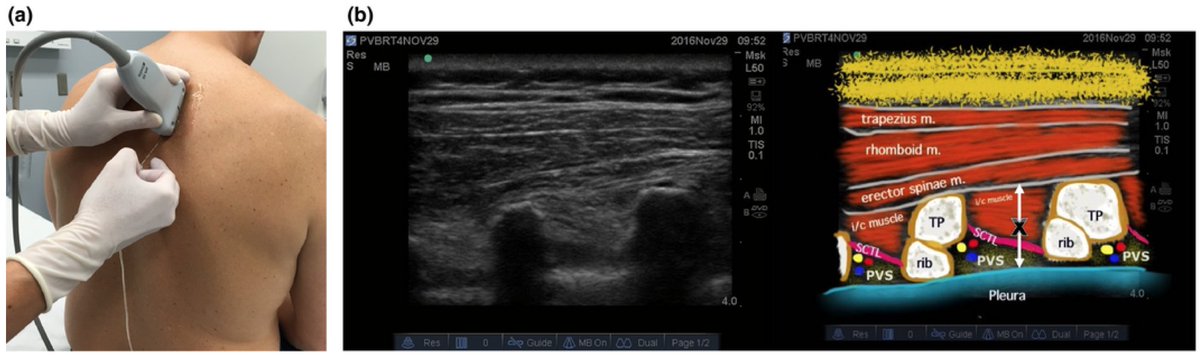


For my single shot blocks, I’m always looking for ways to prolong my regional anesthetic effect. For awhile, Exparel was the most talked about drug to have a 72 hour blockade. We don’t have this medication available to us at the hospital. Therefore, it’s time to get creative and hit the literature to see what has worked for prolonging our blocks.


Other useful links:
After speaking to a colleague of mine regarding regional anesthesia for thoracotomy and mastectomy, I am reading up on Erector Spinae Plane (ESP) block.
**Updated May 2022**
The erector spinae plane block: a narrative review. Korean J Anesthesiol. 2019 Jun; 72(3): 209–220.
Continuous ESP block catheter (my current regimen and what I’m able to get at my institution):